The Closed-Loop Prevention Platform for Value-Based Care
Transform predictive analytics into scalable prevention. Calcium identifies emerging risk, prioritizes intervention, and stabilizes patient health before complications occur.
Calcium: The Closed-Loop Prevention Platform for Value-Based Care
Value-Based Care organizations are increasingly responsible for improving patient outcomes while controlling the total cost of care. Yet many health systems and physician groups still lack the infrastructure needed to detect rising patient risk early enough to prevent costly complications.
The Calcium digital health platform was built to solve this challenge.
By combining predictive intelligence, behavioral monitoring, and digital care pathways, Calcium enables healthcare organizations to identify emerging risk earlier, prioritize clinical attention, and prevent deterioration across large patient populations.
Instead of simply identifying high-risk patients through dashboards and reports, Calcium transforms predictive insight into continuous preventive action.
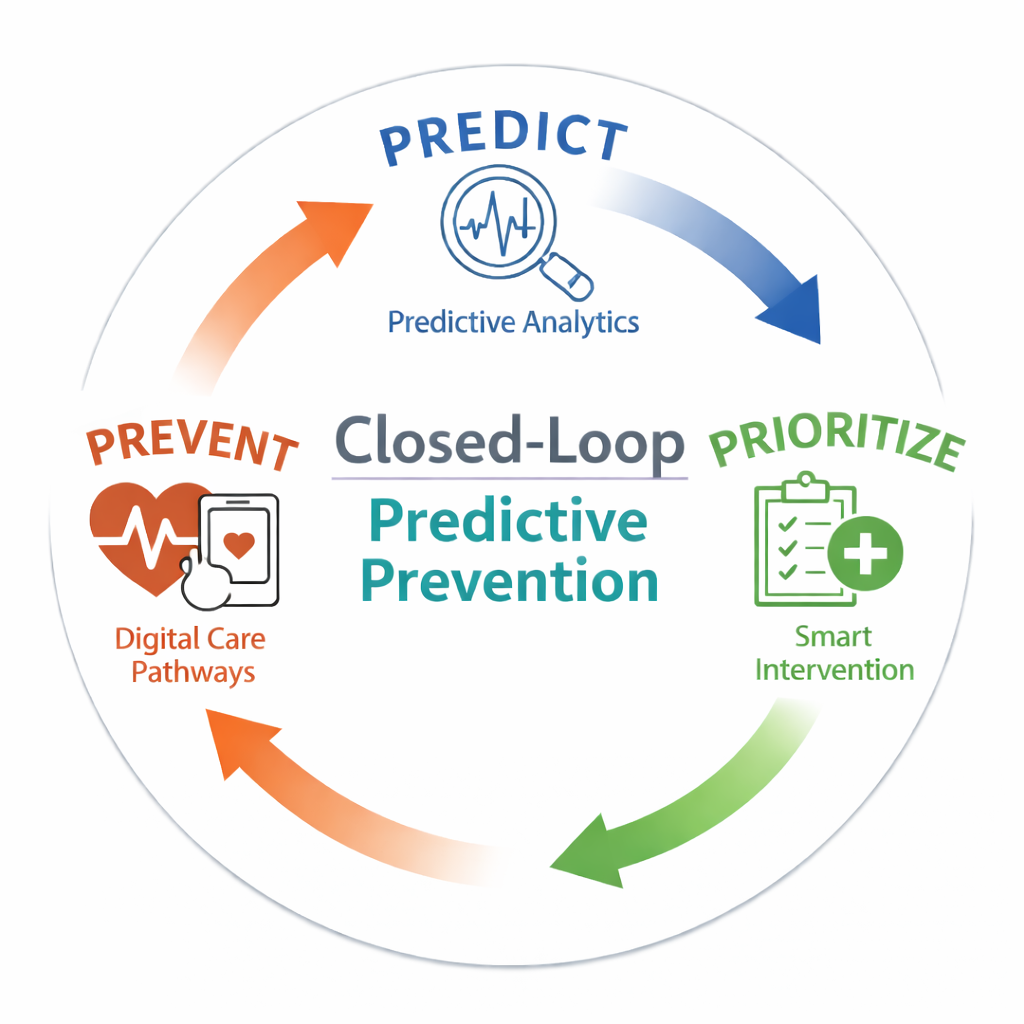
Predict. Prioritize. Prevent.
• Identify rising patient risk earlier
• Guide patients through preventive care pathways
• Enable scalable prevention across large populations
• Reduce avoidable hospitalizations and emergency utilization
Prevention Infrastructure for the Value-Based Care Era
Traditional population health tools can identify high-risk patients, but they often fail to provide the operational infrastructure required to guide patients through preventive behaviors or monitor real-world health signals between clinical visits.
As a result, healthcare organizations frequently face a persistent gap between insight and intervention.
Calcium bridges this gap.
The Calcium platform introduces a new approach to population health infrastructure called Closed-Loop Predictive Prevention. This approach integrates predictive analytics, digital care pathways, behavioral monitoring, and provider escalation workflows into a continuous prevention system.
Rather than reacting to complications after they occur, healthcare organizations can intervene earlier—stabilizing patient conditions before they lead to hospitalizations, emergency department visits, or disease progression.
Why It Matters
Scalable Prevention Is the Foundation of Value-Based Care
Healthcare reimbursement models are rapidly shifting away from fee-for-service payments toward value-based arrangements that reward outcomes rather than volume.
This transition has created new challenges for healthcare organizations responsible for managing population health outcomes.
Workforce Constraints
Traditional care management approaches rely heavily on manual outreach, phone calls, and appointment reminders. While these methods can be effective, they are difficult to scale across thousands of patients.
Care management teams simply cannot maintain continuous engagement with large patient populations without digital infrastructure.
The Prevention Gap
Most Value-Based Care organizations have invested heavily in population health analytics platforms that generate risk stratification reports. However, these systems typically stop at identifying risk rather than operationalizing prevention.
Healthcare organizations know which patients are at risk but they often lack the tools required to prevent deterioration at scale.
Calcium’s Revolutionary Framework
A Closed-Loop Predictive Prevention Platform
Calcium introduces a new infrastructure model designed specifically for Value-Based Care: Closed-Loop Predictive Prevention.
The platform operates through three core actions:
Predict → Prioritize → Prevent
Through this continuous cycle, Calcium enables healthcare organizations to stabilize patient conditions before deterioration occurs.
Predict
Calcium aggregates patient data from multiple sources, including electronic health records, claims systems, medication histories, wearable devices, and patient-reported inputs.
Predictive models analyze these signals to detect early indicators of rising risk.
This allows healthcare organizations to identify patients who may be approaching clinical deterioration before complications occur.
Prioritize
Care teams cannot intervene with every patient simultaneously.
Calcium prioritizes patients based on risk severity, engagement patterns, and predicted outcomes. Care teams receive prioritized dashboards highlighting individuals who require immediate attention.
This ensures that clinical resources are directed toward patients where intervention will have the greatest impact.
Prevent
Digital care pathways guide patients through preventive behaviors and disease management activities between clinical visits.
Continuous monitoring detects deviations in health signals, adherence patterns, and patient engagement. When necessary, alerts escalate to care teams for timely intervention.
The Evolving Landscape
Current Value Based Care Tools Identify Risk, but Fail to Prevent It
The current Value-Based Care technology ecosystem includes several categories of digital health tools. While each category provides valuable capabilities, none fully address the operational challenge of scalable prevention.
Population Health Analytics
Population health platforms aggregate clinical and claims data to generate risk stratification models and performance dashboards.
These systems help organizations understand which patients are likely to incur high healthcare costs. However, analytics tools rarely provide mechanisms for guiding patient behavior or delivering preventive interventions.
Remote Patient Monitoring
Remote monitoring technologies capture physiological data from connected medical devices such as blood pressure monitors or glucose meters.
While these systems provide valuable health signals, many monitoring programs lack coordinated care pathways that translate device data into structured prevention workflows.
Patient Engagement Solutions
Patient engagement applications often focus on communication features such as messaging, reminders, and educational content.
Although engagement tools can improve communication between patients and providers, many lack deep integration with clinical workflows or predictive population health systems.
Risk Adjustment Systems
Risk adjustment tools help healthcare organizations document patient complexity and optimize reimbursement under value-based contracts.
However, these platforms focus primarily on financial reporting rather than clinical prevention.
Together, these systems provide valuable insights but fail to deliver a unified solution for operationalizing prevention across large patient populations.
Challenges & Issues
Healthcare Organizations Struggle to Operationalize Prevention Across Patient Populations
Healthcare organizations operating under value-based payment models face several structural challenges that make prevention difficult to achieve.
Rising Utilization & Cost Pressure
Avoidable hospital admissions, emergency department visits, and complications significantly increase total cost of care under Value-Based Care contracts.
Preventing these events requires earlier detection of risk signals and scalable preventive engagement across patient populations.
Late Detection of Clinical Deterioration
Many Value-Based Care organizations identify patient deterioration only after symptoms worsen or complications occur.
Without continuous monitoring of behavioral and clinical signals, opportunities to intervene earlier and prevent costly health events are frequently missed.
Limited Care Team Capacity
Care management teams must oversee thousands of patients across multiple risk categories.
Manual outreach methods such as phone calls and appointment reminders cannot scale effectively, limiting the ability to provide proactive support across entire patient populations.
Inconsistent Patient Engagement
Sustaining patient engagement between clinical visits remains a persistent challenge.
Many patients struggle to follow care plans, track symptoms, or maintain preventive behaviors without structured digital guidance and continuous feedback from care teams.
Fragmented Patient Data
Patient information is often scattered across multiple electronic health record systems, claims databases, and external providers.
This fragmentation limits visibility into the full patient history, making it difficult to identify emerging risks early and coordinate preventive care.
Lack of Coordinated Prevention Workflows
Many healthcare organizations lack structured digital pathways that guide patients through preventive care activities.
Without standardized workflows, interventions are inconsistent, making it difficult to ensure patients complete recommended screenings, medication regimens, and lifestyle changes.
Delayed Preventive Interventions
Although predictive analytics may identify high-risk patients, many organizations struggle to translate insights into timely interventions.
Without automated prioritization and engagement systems, preventive actions often occur too late to avoid hospitalizations or disease progression.
Difficulty Prioritizing High-Risk Patients
Care teams often struggle to determine which patients require immediate attention.
Without intelligent prioritization tools, clinicians may spend valuable time on lower-risk individuals while patients experiencing rising clinical risk remain unnoticed.
Poor Medication Adherence
Medication adherence remains one of the most common drivers of chronic disease deterioration.
Without structured monitoring, reminders, and patient feedback systems, providers often lack visibility into whether patients are consistently following prescribed treatment regimens.
Transforming Prevention into a Smarter, Scalable Care Model
Value-Based Care organizations face a growing challenge: they must improve patient outcomes and reduce healthcare utilization while managing increasingly complex populations. Yet many healthcare systems still rely on fragmented tools and manual workflows that make it difficult to intervene early enough to prevent costly complications.
The Calcium platform was designed to close this gap. By integrating predictive analytics, digital care pathways, behavioral monitoring, and prioritized clinical workflows, Calcium enables healthcare organizations to move from reactive care to proactive prevention. This closed-loop approach allows providers to detect emerging risk earlier, guide patients through preventive behaviors, and intervene before conditions escalate into hospitalizations or emergency events.

Earlier Detection of Risking Risk
Identifying clinical deterioration before it becomes a crisis is essential for successful Value-Based Care programs. The Calcium platform uses predictive analytics and real-world behavioral signals to detect early warning signs that traditional systems often miss.
By combining clinical data, patient-reported symptoms, and engagement patterns, the platform can highlight patients whose health status may be worsening—even before they require urgent care.
Examples of early risk indicators include:
- Changes in symptom reporting
- Declining medication adherence
- Missed preventive milestones
- Behavioral disengagement from care pathways
These insights allow care teams to intervene earlier, stabilizing patients before complications occur.
Start identifying patient risk earlier with Calcium’s predictive prevention platform. Begin your 30-day free trial today.

Continuous, Automated Patient Engagement
Patient outcomes depend heavily on what happens between clinical visits. Unfortunately, many healthcare organizations struggle to maintain meaningful engagement with patients outside the care setting.
Calcium solves this challenge by delivering structured digital pathways that guide patients through daily health behaviors and preventive care tasks. These pathways provide ongoing reminders, education, symptom tracking, and progress feedback.
Continuous engagement supports:
- Better patient accountability
- Increased adherence to care plans
- Earlier identification of health changes
By maintaining a consistent connection with patients, providers gain a clearer picture of how conditions evolve in real-world settings.
See how continuous engagement improves patient outcomes. Explore Calcium with a 30-day free trial.

Customizable Digital Care Pathways
Care pathways transform clinical guidelines into structured workflows that guide patients step-by-step through preventive and chronic care activities.
Calcium allows healthcare organizations to deploy configurable digital pathways tailored to specific conditions and care programs. These pathways standardize preventive interventions while remaining flexible enough to adapt to individual patient needs.
Common pathway examples include:
- Diabetes management programs
- Heart failure monitoring workflows
- Preventive screening schedules
- Medication adherence reinforcement
By digitizing these care processes, organizations can ensure that preventive interventions occur consistently across entire patient populations.
Discover how digital pathways operationalize prevention. Start your 30-day free trial of Calcium today.

Medication Adherence Support
Medication adherence is one of the most critical drivers of chronic disease stability. Yet many patients struggle to follow complex medication regimens without ongoing support.
Calcium helps providers monitor adherence patterns and reinforce treatment plans through automated reminders, education, and behavioral feedback mechanisms.
The platform enables:
- Medication reminders and adherence tracking
- Patient self-reporting of missed doses
- Alerts when adherence patterns decline
These capabilities allow care teams to intervene quickly when adherence drops, reducing the risk of disease progression and complications.
Strengthen medication adherence across your population. Try Calcium with a 30-day free trial.

Scalable Prevention Across Populations
Traditional care management programs often focus on the highest-risk patients because manual outreach cannot scale across entire populations.
Calcium enables healthcare organizations to extend preventive care to thousands of patients simultaneously through automated monitoring and digital engagement tools.
The platform supports scalable prevention by:
- Automating routine care pathway tasks
- Monitoring engagement across large populations
- Highlighting patients requiring intervention
This allows care teams to allocate resources strategically while ensuring that preventive guidance reaches all patients not just a small subset.
Scale preventive care across your entire population. Start a 30-day free trial of Calcium today.

Real-Time Behavioral Change
Clinical deterioration often begins with subtle behavioral signals long before measurable clinical changes occur. These signals can include reduced engagement with care pathways, missed tasks, or changes in symptom reporting.
Calcium analyzes behavioral patterns to identify early warning indicators that may suggest rising health risk.
Behavioral intelligence insights may include:
- Decreased interaction with care guidance
- Missed preventive activities
- Inconsistent symptom tracking
These signals help providers detect emerging issues earlier and intervene before conditions worsen.
Unlock real-time behavioral insights with Calcium. Experience the platform through a 30-day free trial.

Automated Post-Discharge Recovery Monitoring
The period following hospital discharge is one of the most vulnerable phases in a patient’s care journey. Without structured follow-up, complications can develop quickly and lead to readmissions.
Calcium provides digital recovery pathways that guide patients through post-discharge care while monitoring symptoms and engagement.
These pathways support recovery through:
- Symptom check-ins and recovery tracking
- Medication adherence reminders
- Alerts for concerning symptom patterns
Early detection of complications allows care teams to intervene before readmission becomes necessary.
Improve post-discharge outcomes with proactive monitoring. Try Calcium free for 30 days.

Chronic Disease Stabilization
Chronic diseases such as diabetes, hypertension, and heart failure require continuous management rather than episodic treatment. Calcium helps providers stabilize these conditions through structured monitoring and ongoing behavioral support.
Patients are guided through daily activities that support disease control while providers receive visibility into evolving health trends.
Chronic care capabilities include:
- Condition-specific care pathways
- Symptom monitoring and self-reporting
- Behavioral engagement tracking
By supporting long-term disease management, Calcium helps reduce complications and improve population health outcomes.
Stabilize chronic disease populations with digital prevention tools. Start your 30-day free trial of Calcium.

Prioritized Clinical Workflows
Care teams often face an overwhelming number of patients and tasks. Without intelligent prioritization systems, clinicians may struggle to determine which patients require immediate attention.
Calcium solves this challenge by highlighting individuals whose health signals suggest elevated risk.
The platform enables prioritized workflows through:
- Risk-based patient scoring
- Escalation alerts for emerging issues
- Actionable dashboards for care teams
These tools ensure that clinical attention is directed toward patients most likely to benefit from intervention.
Focus clinical resources where they matter most. Explore Calcium with a 30-day free trial.

Reduced Total Cost of Care
Under Value Based Care contracts, preventable hospitalizations, emergency visits, and complications directly affect financial performance.
By identifying risk earlier and guiding patients through preventive behaviors, Calcium helps healthcare organizations reduce avoidable utilization across large populations.
Key financial impact areas include:
- Lower hospital admission rates
- Reduced emergency department utilization
- Improved chronic disease control
Preventing deterioration before it occurs protects both patient health and organizational financial sustainability.
See how Calcium helps reduce total cost of care. Start your 30-day free trial today.
The Calcium Difference
Many value-based care platforms excel at identifying risk. They aggregate claims, clinical, and utilization data to help healthcare organizations answer a critical question: Which patients are most likely to deteriorate?
But identifying risk alone does not prevent adverse outcomes. Providers must still operationalize interventions across care teams, workflows, and patient engagement channels.
This is where the Calcium platform introduces a fundamental shift. Rather than stopping at analytics and reporting, Calcium translates predictive insights into coordinated care execution activating prevention pathways, intervention workflows, and structured patient engagement. The result is a system that moves from retrospective population health reporting to real-time operational prevention, enabling healthcare organizations to intervene earlier, scale care management efficiently, and reduce avoidable deterioration across large patient populations.
Use Cases
Operationalizing Prevention Across the Patient Care Journey
Healthcare organizations operating under Value-Based Care contracts face a fundamental challenge: they must improve outcomes while controlling costs across large patient populations. Achieving this goal requires more than retrospective analytics or periodic patient outreach. Providers need operational systems that can continuously monitor patient health signals, guide individuals through preventive care behaviors, and escalate intervention when deterioration begins.
The Calcium platform enables healthcare organizations to operationalize prevention through digital care pathways, predictive risk detection, and continuous monitoring. These capabilities translate into practical applications across a wide range of clinical and operational scenarios. The following use cases illustrate how Calcium supports care teams in stabilizing chronic conditions, improving recovery after hospitalization, and proactively managing patient populations before complications occur.
Chronic Disease Stabilization
Chronic disease management is one of the most critical drivers of cost and outcomes in Value-Based Care. Conditions such as diabetes, heart failure, and hypertension require continuous monitoring and behavioral support between clinical visits. Calcium enables care teams to manage these populations more effectively by guiding patients through structured digital care pathways and identifying early signals of deterioration.
Patients receive condition-specific guidance, reminders, and symptom tracking tools that reinforce treatment adherence and lifestyle management. Care teams can quickly identify individuals who require intervention.
Key capabilities include:
- Symptom monitoring and condition-specific check-ins
- Medication adherence tracking and reminders
- Early alerts for worsening symptoms or engagement decline
By stabilizing chronic conditions earlier, organizations can reduce complications, prevent hospitalizations, and improve long-term population health outcomes.
Preventive Screening Completion
Preventive screenings are essential for early detection of serious conditions such as cancer, cardiovascular disease, and metabolic disorders. However, many healthcare organizations struggle to maintain high screening completion rates across large patient populations.
Calcium improves screening adherence by guiding patients through preventive care pathways that include reminders, education, and scheduling prompts. The platform continuously monitors completion status and engagement levels.
Key capabilities include:
- Automated reminders for recommended screenings
- Patient education explaining the importance of preventive care
- Escalation alerts when screenings remain incomplete
This proactive approach helps healthcare organizations improve quality metrics and detect health risks earlier.
Medication Adherence Management
Medication adherence is a persistent challenge for healthcare organizations managing chronic disease populations. Patients may forget to take medications, misunderstand dosing instructions, or stop treatment altogether when symptoms improve.
The Calcium platform helps address these challenges by embedding medication adherence support directly within digital care pathways. Patients receive reminders, educational reinforcement, and structured tracking tools that encourage consistent adherence.
Key capabilities include:
- Medication reminders integrated with care pathways
- Patient-reported adherence tracking
- Behavioral engagement signals that detect declining adherence
When adherence issues are detected, care teams can intervene quickly, preventing complications that often arise from inconsistent medication use.
High Emergency Dept. Utilizer Management
Patients who frequently rely on emergency departments often represent a small segment of the population that generates a disproportionate share of healthcare utilization. These individuals typically have complex health needs, unstable chronic conditions, or limited access to preventive care.
Calcium enables healthcare organizations to proactively manage these high-utilization populations through predictive risk detection and continuous engagement. The platform identifies early warning signals that suggest a patient may be heading toward another emergency visit.
Key capabilities include:
- Predictive identification of high-risk utilization patterns
- Structured preventive engagement pathways
- Care team alerts when deterioration signals emerge
By stabilizing these patients earlier, healthcare organizations can significantly reduce unnecessary emergency department visits.
Post-Discharge Recovery Monitoring
Care Team Prioritization & Workload Optimization
Population health programs often generate large volumes of risk alerts and patient data, making it difficult for care teams to determine where to focus their attention. Without prioritization tools, care managers may struggle to allocate resources effectively.
Calcium addresses this challenge by prioritizing patients based on predictive risk scores, behavioral engagement patterns, and real-time health signals. Care teams receive dashboards highlighting individuals most likely to deteriorate.
Key capabilities include:
- Risk-based patient prioritization dashboards
- Automated alerts for high-risk individuals
- Intelligent workload triage for care managers
This capability allows healthcare organizations to deploy limited clinical resources where they can have the greatest impact on outcomes and cost reduction.
The period immediately following hospital discharge is one of the highest-risk moments in the patient care journey. Many complications and readmissions occur during the first few weeks after discharge when patients are recovering at home without direct clinical supervision.
Calcium addresses this gap by guiding patients through structured post-discharge recovery pathways. These pathways provide daily recovery guidance while collecting symptom data and monitoring behavioral signals that may indicate complications.
Key capabilities include:
- Structured recovery check-ins and symptom reporting
- Medication reminders and recovery instructions
- Escalation alerts for potential complications
This approach allows providers to detect deterioration early and intervene before a situation escalates into a hospital readmission or emergency department visit.
FAQ
1. What is Closed-Loop Predictive Prevention?
Closed-Loop Predictive Prevention is a population health infrastructure model designed to transform predictive insight into real-world clinical action. The framework integrates predictive analytics, digital care pathways, continuous monitoring, and provider escalation workflows into a unified prevention system. Rather than simply identifying which patients are at risk, the system continuously monitors patient data and engagement signals, activates preventive interventions, and alerts care teams when escalation is required. This closed-loop approach ensures that emerging health risks are not merely observed in reports but actively addressed through coordinated care workflows.
2. How does Calcium support Value-Based Care programs?
Calcium supports Value-Based Care programs by enabling healthcare organizations to intervene earlier in the patient care cycle. The platform identifies rising health risks through predictive analytics, prioritizes patients who require attention, and guides individuals through structured digital care pathways designed to stabilize chronic conditions and reinforce preventive behaviors. Continuous monitoring allows care teams to detect changes in patient status before complications occur. By reducing avoidable hospitalizations, emergency department visits, and disease progression, Calcium helps organizations improve clinical outcomes while controlling total cost of care.
3. How does Calcium differ from population health analytics platforms?
Traditional population health analytics platforms focus primarily on reporting and risk stratification. They analyze clinical and claims data to identify patients who are likely to incur high healthcare costs or experience complications. However, these systems typically stop at generating insights. Calcium goes further by operationalizing prevention. The platform transforms predictive insights into structured intervention workflows, digital care pathways, and continuous monitoring systems that actively guide patient behavior and enable earlier clinical intervention.
4. Can Calcium integrate with electronic health records?
Yes. Calcium is designed to integrate with existing electronic health record (EHR) systems and other healthcare data platforms. The system aggregates information from multiple sources, including EHRs, claims databases, medication records, and connected health devices. By consolidating these data streams into a unified patient intelligence layer, Calcium enables healthcare organizations to maintain continuity of care while extending their existing infrastructure with preventive workflows, predictive analytics, and patient engagement capabilities.
5. What patient populations benefit most?
The Calcium platform delivers the greatest impact for patient populations that carry elevated clinical risk or require continuous monitoring outside traditional clinical settings. These groups often include individuals with chronic diseases such as diabetes, heart failure, and hypertension. Additional high-impact populations include patients recovering from hospital discharge, individuals with complex medication regimens, and patients with frequent emergency department utilization. By proactively managing these populations, healthcare organizations can significantly reduce complications and avoidable utilization.
6. How does Calcium detect rising risk?
Calcium detects rising patient risk by combining predictive analytics with continuous monitoring of real-world health signals. The platform analyzes clinical data, medication histories, claims information, behavioral engagement patterns, and data from connected devices such as blood pressure monitors or glucose meters. Machine learning models evaluate these signals to identify early indicators of deterioration, including declining medication adherence, worsening symptoms, or reduced engagement with care pathways. When risk thresholds are reached, alerts are generated to prompt timely intervention.
7. What are digital care pathways?
Digital care pathways are structured, condition-specific workflows designed to guide patients through preventive health behaviors and disease management activities. These pathways combine educational resources, reminders, symptom tracking tools, medication adherence prompts, and behavioral reinforcement strategies. Patients receive step-by-step guidance tailored to their health conditions, while providers gain visibility into patient progress. Digital care pathways help standardize care management across large populations and ensure that patients receive consistent, evidence-based guidance between clinical visits.
8. Can Calcium reduce hospital readmissions?
Yes. Calcium can help reduce hospital readmissions by supporting structured post-discharge recovery monitoring. After a patient leaves the hospital, the platform guides them through recovery pathways that include symptom tracking, medication adherence reminders, and scheduled check-ins. Continuous monitoring allows care teams to detect early warning signs of complications, such as worsening symptoms or declining adherence. When concerning trends emerge, providers are alerted so they can intervene before the condition escalates into a hospital readmission.
9. How does the platform support medication adherence?
Medication adherence is a critical component of chronic disease management and preventive care. Calcium supports adherence through digital reminders, medication tracking tools, and structured engagement pathways designed to reinforce treatment plans. The platform also monitors behavioral signals that may indicate declining adherence, such as missed check-ins or inconsistent engagement with care activities. When potential adherence issues are detected, care teams can intervene with targeted outreach and support.
10. How scalable is the platform?
The Calcium platform is designed to scale across large patient populations while supporting multiple care teams and clinical conditions. Automated workflows, predictive prioritization, and digital care pathways allow organizations to manage thousands of patients simultaneously without dramatically increasing staff workload. This scalability is particularly important for Value-Based Care organizations responsible for managing population health outcomes across Medicare Advantage, Accountable Care Organization (ACO), and risk-bearing provider networks.
11. What types of data does Calcium use?
Calcium integrates a wide range of healthcare data sources to generate a comprehensive view of patient health. These data sources include electronic health records, insurance claims data, medication histories, laboratory results, wearable device data, connected medical device readings, and patient-reported outcomes. Behavioral engagement signals—such as participation in care pathways or symptom reporting—are also analyzed. By combining these data streams, the platform can identify emerging risk patterns and support more proactive care management.
12. How long does implementation take?
Implementation timelines vary depending on organizational size, integration requirements, and deployment scope. In many cases, organizations can begin piloting the platform within several weeks by integrating available data sources and launching digital care pathways for targeted patient populations. Initial pilot programs often focus on high-impact cohorts such as chronic disease populations or post-discharge patients. Once the system demonstrates measurable outcomes, organizations can expand deployment across additional service lines and patient populations.
13. Does Calcium replace population health tools?
No. Calcium is designed to complement existing population health analytics systems rather than replace them. Most healthcare organizations already use analytics platforms to generate risk stratification reports and performance dashboards. Calcium builds on these insights by providing the operational infrastructure required to act on them. The platform translates predictive signals into structured patient engagement, continuous monitoring, and escalation workflows that enable organizations to move from insight to intervention.
14. Can the platform support Medicare Advantage programs?
Yes. Calcium is particularly well suited for healthcare organizations operating under Medicare Advantage contracts and other risk-bearing payment models. These programs require providers to manage the total cost of care while maintaining strong quality metrics across large patient populations. By enabling earlier intervention, continuous patient engagement, and proactive chronic disease management, Calcium helps organizations reduce avoidable utilization and improve performance under value-based reimbursement models.
15. What financial outcomes can organizations expect?
Healthcare organizations implementing Calcium may experience improvements across several key financial metrics associated with Value-Based Care performance. These improvements can include reductions in hospital admission rates, lower emergency department utilization, improved medication adherence, higher preventive screening completion, and reductions in total cost of care per member per month. By preventing complications before they escalate, organizations can improve both clinical outcomes and financial sustainability.
